Welcome to the wild ride through the land of Chronic diseases, where the only thing more persistent than your neighbor’s unsolicited advice is the quest for health! Here, we’ll unravel the mysteries of those sneaky, long-term ailments that like to crash the party and stay way too long, making us rethink our late-night pizza choices. Buckle up as we dive into how these ailments impact not just the individual but society at large, and why our lifestyle choices can either be the magic wand or the poison apple in this health narrative!
Chronic diseases are not just medical jargon; they’re the uninvited guests at our health shindig, often resulting from lifestyle choices and environmental factors. From diabetes to multiple sclerosis, each condition tells a compelling story of resilience and management, reminding us that with the right effort and support, we can turn the tables on these chronic companions!
Chronic Diseases Overview
Chronic diseases are like that uninvited guest at a party who just won’t leave. They stick around for years, sometimes decades, and can seriously mess with your fun. Understanding chronic diseases is crucial because they affect millions of people globally and have a significant impact on healthcare systems and economies. It’s not just about the individual suffering; it’s a collective concern that can bring society to its knees—much like a bad dance move gone wrong.Common types of chronic diseases include heart disease, diabetes, cancer, asthma, and arthritis.
These diseases are not just personal battles; they create widespread social challenges. For instance, heart disease is the leading cause of death worldwide, and its prevalence can lead to increased healthcare costs and reduced productivity in the workforce. According to the World Health Organization, chronic diseases are responsible for 71% of all deaths globally, making them a significant public health concern that no one can afford to ignore.
Impact of Lifestyle Choices
Lifestyle choices play a pivotal role in the development of chronic diseases, often acting as a double-edged sword. The decisions we make daily—what we eat, how much we move, our stress levels, and even our sleep habits—can either pave the way to a healthy life or lead us down a slippery slope of chronic ailments. Consider the following lifestyle factors and their connection to chronic diseases:
- Diet: Consuming a diet high in processed foods, sugars, and unhealthy fats can increase the risk of conditions like type 2 diabetes and heart disease. Think of your plate as a long-term investment; choose wisely for a healthy return!
- Physical Activity: Regular exercise is like a superhero cape for your body, fighting off diabetes and heart disease. The CDC recommends at least 150 minutes of moderate-intensity exercise each week to keep chronic diseases at bay. No gym required; even a brisk walk counts!
- Smoking: Smoking is like playing a game of Russian roulette with your health. It increases the risk of cancers, heart disease, and respiratory issues. Breaking free from tobacco can add years to your life—a far better prize than any smoke break.
- Alcohol Consumption: While a glass of wine can be good for the heart in moderation, excessive drinking is a one-way ticket to liver problems and other chronic diseases. Moderation is the key—think of it as a balancing act at a circus!
- Stress Management: Chronic stress acts like a sneaky thief, stealing not just your joy but also your health. Practices like meditation, yoga, or even taking a moment to laugh can help mitigate its effects and keep chronic diseases at bay.
As we can see, our daily choices can create a ripple effect on our health, either promoting wellness or paving the way for chronic disease. The journey to better health starts with each individual making informed lifestyle choices—not just for themselves but for the collective well-being of society.
Health and Diabetes
When it comes to chronic diseases, diabetes is like that one friend who just won’t leave the party. Not only is it a major issue on its own, but it also loves to mingle with other chronic conditions, such as heart disease, obesity, and kidney problems. This relationship can be complicated, and much like trying to untangle headphone wires, it requires a bit of understanding and patience.The interplay between diabetes and other chronic diseases is significant.
For instance, individuals with diabetes are at a higher risk of developing cardiovascular diseases, with studies indicating that they are two to four times more likely to experience heart issues than non-diabetics. Additionally, diabetes can lead to kidney damage, commonly known as diabetic nephropathy, and increase the risk of stroke. The complex nature of these relationships highlights the importance of effective disease management and prevention strategies.
Management of Diabetes through Diet and Exercise
Managing diabetes effectively involves a holistic approach that includes a balanced diet and regular physical activity. These lifestyle choices not only help in controlling blood sugar levels but also reduce the risk of complications related to diabetes. Here are some insights into dietary practices and exercise routines that can make living with diabetes a bit more manageable:Maintaining a healthy diet is crucial.
A well-balanced meal plan rich in whole grains, lean proteins, healthy fats, and plenty of fruits and vegetables can work wonders. Consider the following points:
- Carbohydrate Monitoring: Being mindful of carbohydrate intake can help keep blood sugar levels stable. Incorporate complex carbs like quinoa and whole grains, instead of simple sugars.
- Portion Control: Eating smaller portions more frequently can help manage hunger and blood sugar levels.
- Hydration Matters: Staying hydrated is vital. Water is the best choice for hydration, while sugary drinks should be avoided.
Exercise plays a vital role in managing diabetes, as it helps improve insulin sensitivity and can lower blood sugar levels. Engaging in regular physical activity can be a game-changer. Here are some types of exercises beneficial for diabetes management:
- Aerobic Activities: Activities like walking, cycling, and swimming can be great for heart health and blood sugar control.
- Strength Training: Lifting weights or bodyweight exercises can increase muscle mass, which is beneficial for glucose metabolism.
- Flexibility and Balance: Yoga or stretching exercises can enhance balance and flexibility, helping prevent injuries.
With diabetes prevalence on the rise, it’s crucial to address its impact on public health. According to the International Diabetes Federation, approximately 537 million adults were living with diabetes in 2021, and this number is projected to reach 643 million by 2030. The economic burden is also significant, with global healthcare expenditures on diabetes projected to reach 966 billion dollars.
This underscores the urgent need for public health initiatives aimed at prevention and management.
“A healthy lifestyle is not just about diet and exercise; it’s about creating a sustainable way of living that promotes well-being in the long run.”
Health and Disability
Chronic diseases and disabilities are like those uninvited guests at a party who refuse to leave, even when the fun is all gone. They can sneak up on you, causing long-term health issues that may limit your physical or mental abilities. Understanding how these conditions intertwine is crucial for both individuals affected and their support networks.Chronic diseases such as arthritis, multiple sclerosis, and diabetes can lead to disabilities that affect daily functioning.
These conditions may limit mobility, decrease stamina, and impair cognitive abilities. For instance, a person with severe arthritis may find it challenging to perform simple tasks like buttoning a shirt or opening a jar—activities we often take for granted. Such limitations can lead to feelings of frustration and isolation, making it essential to address not only the physical but also the emotional aspects of living with chronic conditions.
Impact of Chronic Diseases on Daily Living
The impact of chronic diseases on an individual’s daily life can be profound and multifaceted. Understanding these effects can help in developing better support systems. Consider the following key points:
- Mobility Issues: Chronic diseases can severely limit mobility, making it difficult to navigate everyday environments such as workplaces or homes.
- Fatigue: Many chronic conditions come with fatigue that feels like dragging a boulder uphill. This can hinder motivation and energy for daily tasks.
- Social Isolation: The inability to participate in social activities can lead to feelings of loneliness, which can compound mental health issues like depression.
- Cognitive Challenges: Some chronic diseases, such as diabetes, can affect cognitive functions, making it harder to concentrate or remember things.
Support systems play a pivotal role in managing these challenges. Having a reliable network can make the journey less daunting and more manageable.
Importance of Support Systems
Support systems can be the difference between thriving and merely surviving for individuals with chronic disabilities. These systems often include family, friends, healthcare providers, and community resources. Here’s why they matter:
- Emotional Support: A listening ear can work wonders. Emotional backing from loved ones can help alleviate feelings of frustration and anxiety.
- Practical Assistance: Having someone to help with daily chores can significantly improve quality of life. Imagine having a friend who’s always ready to tackle that mountain of laundry or run errands!
- Access to Resources: Support systems often point individuals toward local resources, helping them navigate healthcare services, therapy options, and financial assistance programs.
- Shared Experiences: Connecting with others facing similar challenges can foster a sense of community and belonging, reducing feelings of isolation.
Resources and Programs for Managing Health and Disability
Navigating health and disability management can feel like wandering through a maze. Fortunately, there are numerous resources and programs designed to provide assistance:
- National Institutes of Health (NIH): Offers extensive research and resources on chronic diseases and disabilities to help individuals better understand their conditions.
- Local Health Departments: Often provide programs tailored to managing chronic diseases, including nutritional guidance, exercise programs, and health screenings.
- Support Groups: Both in-person and online support groups can connect individuals with others facing similar health challenges, providing a platform for sharing experiences and advice.
- Disability Services: Organizations like the Social Security Administration (SSA) offer programs and benefits for those disabled by chronic conditions, ensuring financial support during tough times.
“You don’t have to struggle alone. With the right support and resources, living well with a chronic illness is not just a dream—it’s a possible reality!”
Health and Diseases
Chronic diseases are the uninvited guests at the party of life, sticking around longer than we’d like and making everything a bit less fun. They come with a list of demands that includes regular medication, lifestyle changes, and at times, an entirely new way of looking at life. Let’s dive into the most common chronic diseases, how to keep them at bay, and some success stories that might just inspire you to dance your way out of despair.
Overview of Common Chronic Diseases
Chronic diseases like an unrelenting sitcom character, appear on the health scene, often without an exit strategy. The most prevalent chronic diseases include:
- Heart Disease: The leading culprit, stealing the spotlight in cardiovascular drama.
- Diabetes: Known for its sweet tooth, it plays tricks on blood sugar levels.
- Chronic Respiratory Diseases: Asthma and COPD add some wheezy notes to the script.
- Cancer: A complex plot twist that affects various organs and tissues.
- Obesity: The heavy-weight contender, often linked to other chronic conditions.
These chronic conditions collectively make up a significant portion of health-related challenges, painting a picture that is all too familiar in our modern world.
Preventive Measures for Chronic Diseases
An ounce of prevention is worth a pound of cure, or as we like to say, it’s cheaper than a lifetime supply of medications! Here are vital preventive measures to keep chronic diseases from crashing your health party:
- Regular Exercise: A fun way to kick those calories to the curb—you don’t need to run a marathon, just dance like no one’s watching!
- Balanced Diet: Incorporating fruits, veggies, and whole grains while keeping the junk food at bay can be a tasty endeavor.
- Regular Check-Ups: A yearly health screening is like an annual festival for your body—it’s always good to check the lineup!
- Avoid Tobacco and Limit Alcohol: Time to throw away the cigarettes and sip in moderation; your body will thank you!
- Stress Management: Mindfulness, yoga, or even a good laugh can reduce stress and keep your health in check.
These measures can help keep chronic diseases at bay, allowing you to strut your stuff with confidence and vitality!
Case Studies of Successful Management of Chronic Diseases
Success stories are the glittering gems that shine through the cloud of chronic diseases, proving that with the right approach, one can turn the tide. Here are a few inspiring examples:
- John’s Heart Health Journey: After being diagnosed with heart disease, John embraced a Mediterranean diet and started jogging. Fast forward a year, and he’s not only lost weight but also completed a 5K run—chest bumping his cardiologist!
- Maria’s Diabetes Transformation: Maria learned to count carbs and embraced a low-sugar lifestyle, leading to her reducing insulin dependency. She’s now the neighborhood’s go-to for healthy dessert recipes.
- Tom’s Asthma Control: By practicing breathing exercises and avoiding triggers, Tom transformed from an asthma-prone individual to a weekend hiking enthusiast, conquering trails he once avoided.
These case studies exemplify that chronic diseases don’t have to dictate your life; with determination and proper management, one can reclaim their health and live vibrantly.
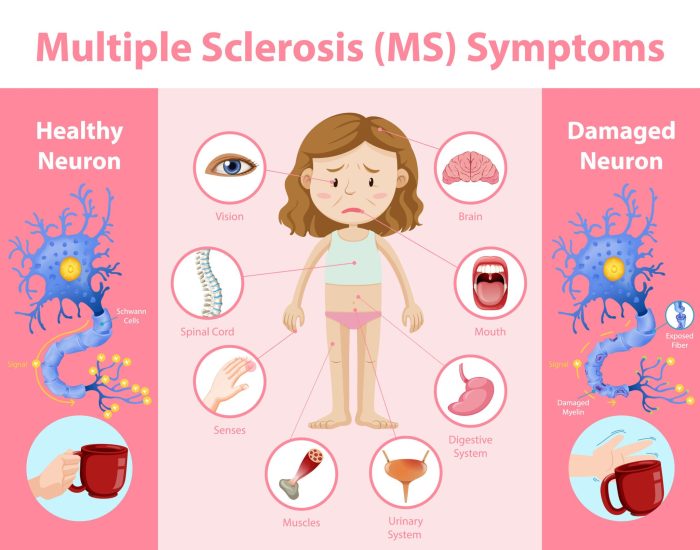
Multiple Sclerosis
Multiple sclerosis (MS) is like an uninvited party crasher at your nervous system’s shindig—showing up unannounced and causing chaos. It’s a chronic disease that disrupts the communication between your brain and body, leading to a variety of symptoms that can vary from person to person. Living with MS can often feel like trying to dance with two left feet while juggling, but understanding the symptoms and challenges can help you manage this condition more effectively.The symptoms of multiple sclerosis can be as unpredictable as a cat on a Roomba.
Common manifestations include fatigue, difficulty walking, numbness or tingling in limbs, vision problems, and muscle stiffness. There might also be cognitive challenges, like memory lapses that can turn everyday tasks into a scavenger hunt for your own thoughts. Individuals with MS often face mobility issues and may experience emotional changes, such as depression and anxiety, which can turn the simplest routines into Herculean feats.
In this rollercoaster of symptoms, every day can feel different, which makes planning rather tricky!
Treatment Options and Lifestyle Adjustments
Managing multiple sclerosis involves a multifaceted approach that combines medical treatments and lifestyle adjustments. While there is no cure for MS, various treatment options are available that can help manage symptoms and slow the disease’s progression. Medications prescribed may include disease-modifying therapies (DMTs) that aim to reduce the frequency and severity of attacks, as well as corticosteroids to manage flare-ups.
On the lifestyle side, embracing healthy habits can significantly improve overall well-being. Here are some strategies that can be helpful:
- Regular exercise: Engaging in physical activity helps maintain mobility and strength, with activities like yoga or swimming often being gentle yet effective.
- Balanced diet: A nutritious diet rich in fruits, vegetables, lean proteins, and healthy fats can help reduce inflammation and improve energy levels.
- Stress management: Techniques such as mindfulness, meditation, or even a good old-fashioned laugh can help alleviate stress that might worsen symptoms.
- Sleep hygiene: Prioritizing quality sleep is essential for coping with fatigue and cognitive challenges common in MS.
Incorporating these adjustments can create a supportive environment for managing MS and enhancing the quality of life.
Support Networks and Resources
Navigating the complexities of multiple sclerosis is made easier with the right support networks and resources. Connecting with fellow individuals affected by MS can provide a wealth of shared experiences, advice, and camaraderie that is crucial for emotional support. There are numerous organizations dedicated to supporting those with MS, which can offer valuable resources such as educational materials, financial assistance, and community events.
Notable networks include:
- National Multiple Sclerosis Society: This organization provides a plethora of resources, including information on local support groups, educational programs, and research initiatives.
- MS Foundation: Aimed at raising awareness and funding research, the MS Foundation offers educational materials and connects individuals with resources.
- Local MS Support Groups: Many communities have local groups that meet regularly for discussions, activities, and support, creating a welcoming environment for sharing experiences.
In addition, online forums and social media groups can serve as interactive platforms where individuals can connect, share advice, and even indulge in some light-hearted banter about their daily challenges with MS. Remember, while MS may be a formidable foe, you’re not alone in this battle; there’s a whole community out there ready to cheer you on and share their wisdom!
Diseases
Chronic diseases are known to be the uninvited guests that stay too long, but let’s not forget about their sneaky counterparts: STDs. These pesky infections don’t just make for awkward conversations; they can leave lasting impacts on health. Buckle up as we explore the long-term effects of untreated STDs, ways to avoid their embrace, and some eye-opening statistics that emphasize the importance of safe practices.
Long-term Effects of Untreated STDs
Untreated STDs can be like a bad credit score: they can haunt you long after the initial incident. The repercussions can range from mild inconveniences to severe health complications. Here are some notable consequences of ignoring these infections:
- Fertility Problems: Infections like chlamydia and gonorrhea can cause pelvic inflammatory disease (PID), which might lead to infertility in both men and women.
- Chronic Pain: Conditions such as PID can result in debilitating pelvic pain that refuses to take a hint.
- HIV Risk: Certain STDs can increase the likelihood of acquiring or transmitting HIV, making untreated STDs a double whammy.
- Organ Damage: Some STDs can cause irreversible damage to organs, including the heart and liver, leading to more serious health issues over time.
- Pregnancy Complications: Pregnant individuals with untreated STDs can face serious risks, including premature birth and low birth weight.
Preventive Measures and Safe Practices
Preventing STDs is not just about avoiding the awkward chat; it’s about safeguarding your health and future. Here are effective measures to reduce the risk of transmission:
- Condom Use: Latex condoms are your best friends; they significantly reduce the risk of STD transmission when used consistently and correctly.
- Regular Testing: Getting tested regularly is like taking your car for maintenance; it helps catch problems early before they escalate.
- Know Your Partner: Having open and honest conversations with partners about sexual health can be a game-changer.
- Limit Partners: Reducing the number of sexual partners lowers the odds of encountering an STD—think of it as a VIP guest list for your health.
- Vaccination: Vaccines are available for diseases like HPV and hepatitis B. They act like an umbrella, protecting you from potential downpours.
Statistics on STD Prevalence
Understanding the prevalence of STDs can illuminate the impact they have on public health. Here are some staggering statistics that underline the urgency of addressing STDs:
- Global Reach: According to the World Health Organization, more than 1 million STDs are acquired every day worldwide, showcasing the need for widespread education and preventive measures.
- Youth Vulnerability: Nearly half of all new STDs occur in individuals aged 15-24, making this age group particularly susceptible to infections.
- Chlamydia Explosion: The CDC reported over 1.8 million cases of chlamydia in the United States in 2019, emphasizing the ongoing epidemic.
- Syphilis Resurgence: In recent years, syphilis rates have soared by over 70% in the U.S., signaling a troubling trend that requires immediate attention.
- Health Implications: The financial burden of STDs on the U.S. healthcare system is more than $16 billion annually, highlighting the economic impact of these infections.
Drug Abuse
Drug abuse is a sneaky little gremlin lurking in the shadows of public health, often leading to chronic diseases that can disrupt lives faster than a cat on a hot tin roof. It’s like trying to juggle flaming swords while riding a unicycle – dangerous, chaotic, and bound to end badly. Understanding the connection between drug abuse and chronic diseases is crucial, as it can have a domino effect that knocks down not just individuals, but entire communities.The relationship between drug abuse and chronic diseases is as tangled as spaghetti at a family dinner.
Substances like alcohol, opioids, and stimulants can exacerbate existing health issues or lead to new ones, including heart disease, liver problems, and mental health disorders. People caught in the crossfire of addiction often find their immune systems weakened, making them more susceptible to infections and other illnesses. It’s a vicious cycle, with drug abuse creating a perfect storm for chronic health problems to flourish.
Rehabilitation and Support Approaches
Rehabilitation for those affected by drug abuse is akin to giving a superhero a makeover – it’s all about restoring their powers and helping them save the day! Various approaches are employed to help individuals reclaim their lives, blending medical, therapeutic, and holistic strategies that work together like a well-oiled machine.Key strategies for rehabilitation include:
- Detoxification Programs: The first step, like removing the battery from a smoke detector, helps clear the body of harmful substances.
- Cognitive Behavioral Therapy (CBT): This nifty tool teaches individuals to change negative thought patterns and behaviors, much like a mental reset button.
- Support Groups: Peer support is invaluable. Groups such as Alcoholics Anonymous allow individuals to share experiences and strategies, creating a community stronger than the sum of its parts.
- Medication-Assisted Treatment (MAT): Medications can help reduce cravings and withdrawal symptoms, allowing individuals to focus on recovery instead of their cravings.
- Holistic Approaches: Yoga, meditation, and art therapy can support emotional healing while giving participants a chance to express themselves creatively.
The importance of these approaches cannot be overstated, as they provide a comprehensive structure for recovery that addresses both the physical and mental aspects of addiction.
Impact of Drug Abuse on Public Health
The statistics surrounding drug abuse are as alarming as a tornado siren on a sunny day. According to the National Institute on Drug Abuse, drug overdose deaths were over 70,000 in the U.S. in 2019 alone, a number that continues to rise. This staggering figure represents not just lost lives, but also a significant drain on public health resources.Consider the financial implications: drug abuse costs the U.S.
healthcare system over $740 billion annually, factoring in healthcare expenses, lost productivity, and crime-related costs. It’s as if drug abuse has set up shop with “open for business” signs flashing everywhere, siphoning off community resources and leaving chronic health issues in its wake.The message is clear: drug abuse is not merely a personal issue but a public health crisis that requires collective action.
Tackling this challenge is like trying to put out a fire while juggling chainsaws – it needs careful planning, strategic support, and a community dedicated to recovery.
Ears
When it comes to aging and chronic diseases, our ears often get overlooked, much like that forgotten piece of fruit at the back of the fridge. But let’s face it, hearing health is crucial—as vital as ensuring your remote control isn’t stuck between the couch cushions. With age, various hearing disorders may creep in, but fear not! The world of hearing health is full of innovative treatments that can help keep you tuned into the sounds of life.As we age, several common hearing disorders can arise, often linked to chronic diseases.
These include presbycusis (the fancy term for age-related hearing loss), tinnitus (ringing in the ears that’s more annoying than a catchy jingle), and noise-induced hearing loss, which can be a result of those years of attending loud concerts or, dare we say, family gatherings. These disorders can severely impact one’s quality of life, making it essential to understand their causes and seek out solutions.
Common Hearing Disorders Associated with Aging and Chronic Diseases
It’s important to recognize the leading culprits of hearing loss, especially as we gracefully age. Here’s a brief rundown of the most common conditions:
- Presbycusis: The gradual loss of hearing due to aging, often affecting high-frequency sounds first, like your grandkids’ laughter or the kettle whistling.
- Tinnitus: A condition that causes persistent ringing or buzzing in the ears, often triggered by prolonged exposure to loud noises, which can drive anyone batty.
- Otitis Media: An infection or inflammation in the middle ear, commonly seen in older adults, occasionally caused by allergies or chronic respiratory issues.
- Noise-Induced Hearing Loss: Damage to the inner ear from loud sounds, which might make you wish you had taken those earplugs seriously all those years ago.
- Barotrauma: Ear pain resulting from changes in air pressure, like when you’re on a flight or deep-sea diving, reminding you to always chew gum on an airplane!
Maintaining hearing health is key, and like any good recipe, it requires the right ingredients. A proactive approach can help preserve your auditory functions, including regular hearing check-ups, avoiding excessive noise exposure, and, when necessary, using hearing protection.
Treatment Options and Preventive Measures for Maintaining Hearing Health
Taking charge of your hearing health is like tuning an instrument—regular maintenance is essential for optimal performance. Here are some ways to keep your ears in tip-top shape:
- Regular Hearing Tests: Think of these as your ears’ version of a routine oil change. Regular check-ups can catch issues early, preventing further damage.
- Hearing Aids: These little wonders amplify sounds, making it easier to hear conversations without straining. You can choose from discreet models that fit snugly in the ear or more traditional styles, depending on your flair.
- Cochlear Implants: For those with severe hearing loss, these surgically implanted devices can provide a sense of sound to people who are profoundly deaf or severely hard of hearing.
- Sound Therapy: Using white noise or other soothing sounds can help mask tinnitus and make you feel a little less like you’re in a never-ending concert of buzzing.
- Ear Protection: Wearing earplugs at loud events or when using power tools can be a game-changer, preserving your precious hearing for years to come.
Emerging Technologies for Hearing Enhancement
As technology advances at lightning speed, so does our ability to enhance hearing. Not just your granddad’s hearing aids anymore, these modern marvels come equipped with sophisticated features that can change the sound game entirely:
- Smart Hearing Aids: These tech-savvy devices connect to smartphones via Bluetooth, allowing users to adjust settings through an app—because who doesn’t want to fine-tune their hearing experience like adjusting their Spotify playlist?
- Bone-Conduction Devices: These innovative gadgets transmit sound through the bones of the skull, allowing individuals with certain types of hearing loss to enjoy their favorite tunes without conventional headphones.
- Augmented Reality Hearing Aids: Merging the realms of virtual reality and auditory assistance, these devices enhance environmental sounds while filtering out background noise, making conversations in crowded places a breeze.
- AI-Driven Sound Processing: Devices equipped with artificial intelligence can analyze the listening environment and automatically adjust settings for optimal clarity—like having a personal sound technician right in your ear!
With these advancements, the future looks bright for those looking to enhance their hearing. By staying informed and proactive, you can ensure that you never miss a beat—whether it’s the latest gossip or that irresistible jingle from your favorite snack commercial.
Eating Disorders
Eating disorders are like that pesky sock that disappears in the dryer; they sneak up on individuals, entwining themselves with chronic diseases in a way that’s often overlooked. While each eating disorder is a unique monster of its own, they frequently emerge alongside chronic diseases, creating a complex web of challenges that can make anyone’s head spin faster than a merry-go-round.
These disorders not only affect physical health but can also exacerbate existing chronic conditions, compelling us to delve deeper into this multifaceted relationship.The connection between eating disorders and chronic diseases can be as intricate as a spaghetti junction. Individuals battling chronic illnesses may develop unhealthy eating habits as a misguided attempt to control their health, stemming from feelings of helplessness or anxiety.
For instance, someone with diabetes might swing between binge eating and restrictive dieting, trying to navigate their dietary needs while battling cravings. This rollercoaster ride can lead to nutritional deficiencies, further complicating their health status and creating a vicious cycle.
Strategies for Overcoming Eating Disorders
Developing a robust toolkit of strategies is crucial for anyone looking to kick eating disorders to the curb. The following methods can pave the way to healthier eating habits and restore balance—like finding that missing sock in the laundry:
- Seek Professional Help: Engaging a nutritionist or therapist can provide tailored guidance. They help in addressing underlying emotions and creating a sustainable eating plan that doesn’t feel like a punishment.
- Mindful Eating: This technique emphasizes savoring each bite and tuning into hunger cues rather than mindlessly munching. Imagine enjoying a piece of chocolate as if it were a fine wine—appreciating every flavor note!
- Create a Balanced Meal Plan: Incorporate a variety of foods. Think of your plate as a colorful palette—more colors mean more nutrients and a happier you!
- Build a Support Network: Surround yourself with friends, family, or support groups. Sharing experiences not only lightens the load but also offers a treasure trove of wisdom and encouragement.
- Set Realistic Goals: Small, achievable goals pave the way for success. Rather than aiming for a complete overhaul overnight, consider making one small change each week!
Support Systems for Individuals Struggling with Eating Disorders
Support systems can act as life jackets in the tumultuous sea of eating disorders, providing individuals with the buoyancy they need to navigate their recovery. These systems can include:
- Professional Counseling: Access to psychologists or counselors trained in eating disorders can offer the emotional support necessary for recovery.
- Support Groups: Gathering with others who share similar experiences fosters understanding and solidarity, making the journey feel less lonely.
- Family Involvement: Family should be encouraged to participate actively, learning about the disorder and ways to support their loved one without judgment.
- Online Resources: Websites and forums dedicated to eating disorder recovery can provide valuable information, community support, and additional resources.
- Healthcare Team Coordination: A team approach involving doctors, dietitians, and therapists ensures comprehensive care tailored to the individual’s needs.
“Recovery from an eating disorder isn’t a linear path; it’s more of a dance, with steps forward and back—but every step counts!”
Navigating the complexities of eating disorders and their intersection with chronic diseases requires resilience, courage, and a solid support system. By arming oneself with knowledge and strategies, it becomes possible to reclaim a healthy relationship with food and body image, proving that even the toughest battles can be won with the right tools and support.
Health and Eczema
Eczema, a chronic skin condition that likes to crash the party without an invite, is all about those itchy, red patches that can do a tap dance on your nerves. If you’ve ever felt like a walking scratch-and-sniff sticker, you’re not alone. Understanding how to manage this unpredictable guest can help you regain control of your skin so it can finally stop demanding attention at the most inconvenient times.Managing eczema requires a ninja-like approach to identifying triggers and implementing preventive measures.
Common culprits often include allergens, irritants, and even the weather—yes, Mother Nature can be fickle! Keeping a journal to track flare-ups can help you pinpoint what sets your skin off. For example, a cozy evening with a glass of red wine might sound delightful, but for some, it could lead to a night of relentless itching.
Understanding Triggers and Preventive Measures
To keep eczema flare-ups at bay, it’s essential to recognize and avoid its notorious triggers. Here’s a list of the usual suspects that might be wreaking havoc on your skin:
- Irritants: Soaps, detergents, and even certain fabrics can irritate sensitive skin.
- Allergens: Pollen, pet dander, and dust mites are like party crashers for eczema.
- Climate: Extreme temperatures, humidity, or dryness can make your skin feel like it’s auditioning for a horror movie.
- Stress: Emotional roller coasters tend to manifest as skin havoc; your mind and skin are more connected than you think!
Preventing flare-ups involves a few lifestyle adjustments. Moisturizing daily is a must—think of it as giving your skin a drink of water. Look for creams and ointments that are fragrance-free and hypoallergenic. A daily routine of applying moisturizer can help keep the skin barrier strong and hydrated. Additionally, wearing breathable fabrics like cotton and avoiding hot showers can help you stay comfortable and itch-free.
Treatment Options and Lifestyle Adjustments
When it comes to treatment options, there are a variety of methods to choose from, each with its charm. Finding the right combination can make a world of difference:
- Topical Steroids: Think of these as the superheroes of the eczema world, swooping in to reduce inflammation and soothe the skin.
- Topical Calcineurin Inhibitors: Non-steroidal creams that help calm down those pesky patches without the side effects of steroids.
- Antihistamines: If your skin feels itchy enough to throw a tantrum, these can help ease the sensation. Just be careful—some may make you drowsy!
- Phototherapy: For the more adventurous, exposing the skin to controlled UV light can help reduce flare-ups.
In addition to medical treatments, daily lifestyle adjustments can play a pivotal role in managing eczema. Regular bathing in lukewarm water, followed by immediate moisturizing, creates a protective layer on the skin. Keeping your nails trimmed short can help prevent skin damage from scratching, while wearing gloves during cleaning tasks can shield your hands from irritants.
“Managing eczema is like a dance; it requires practice, patience, and an occasional twirl to keep your skin happy!”
By adopting these strategies and being mindful of how your skin reacts to different influences, you can turn down the volume on eczema’s disruptive antics and enjoy a more comfortable life in your own skin.
Emotional Freedom Technique
In the grand circus of chronic diseases, where stress often plays the ringleader, Emotional Freedom Technique (EFT) steps in as your trusty juggler, deftly balancing emotions and physical health. This quirky yet effective method taps into the body’s energy meridians—think of it as acupressure for the soul—while you tap your way to emotional liberation and improved health. With a sprinkle of humor, let’s explore how this technique can help you kick chronic conditions to the curb, or at least give them a good nudge.EFT operates on the premise that negative emotions contribute to physical ailments.
By tapping on specific meridian points while focusing on your emotional disturbance, you can help release the blockages that lead to distress. Picture it as giving your emotional baggage a good shake, releasing the cobwebs of anxiety and pain. The benefits of EFT are as diverse as the toppings on a pizza, including reduced stress, improved mental clarity, and even relief from physical symptoms associated with chronic diseases.
Principles and Benefits of Emotional Freedom Technique
The principles behind EFT are rooted in the understanding of energy flow within the body and how it can affect our mental and physical health. Let’s take a look at some of the key components that make this technique so beneficial:
- Energy Meridians: EFT targets specific energy pathways in the body, akin to tuning a musical instrument to achieve harmony.
- Mind-Body Connection: Recognizes the profound link between emotional distress and physical ailments, suggesting that relieving one can positively impact the other.
- Self-Help Tool: Empowers individuals to take charge of their emotional health, making it a cost-effective solution for managing chronic diseases.
- Quick Relief: Many users report feeling immediate effects post-session, like a breath of fresh air after being underwater.
- Versatile Application: Useful for a range of conditions, from stress and anxiety to chronic pain and beyond—like a Swiss army knife for your emotional toolkit.
“The greatest discovery of my generation is that a human being can alter his life by altering his attitudes.” – William James
Several personal testimonies underscore the effectiveness of EFT. For instance, a study involving patients with chronic pain revealed that those who practiced EFT experienced significantly reduced pain levels and improved quality of life. One participant, a retired teacher, shared that after a few weeks of tapping, she could finally enjoy her garden without being sidelined by discomfort—talk about blooming where you’re planted!
Guidelines for Practicing Emotional Freedom Technique
Getting started with EFT is as easy as pouring yourself a cup of herbal tea—no fancy equipment required! Follow these simple guidelines to tap into your emotional freedom:
- Identify the Issue: Focus on what’s bothering you; it could be anything from a looming deadline to an ongoing health condition.
- Rate the Intensity: On a scale of 0 to 10, how intense is your emotional disturbance? This will help track your progress.
- Set Up Statement: Create a phrase that acknowledges the problem and affirms self-acceptance. For instance, “Even though I feel this pain, I deeply and completely accept myself.”
- Start Tapping: Gently tap on the designated meridian points while repeating your setup statement. Key points include the side of your hand, top of your head, eyebrows, under the eyes, and collarbone.
- Reassess Intensity: After a round of tapping, rate your emotional intensity again. Celebrate any decrease—every point counts!
By incorporating EFT into your self-care routine, you’re not only addressing emotional hurdles but also empowering yourself to tackle chronic diseases with a new level of resilience. So grab your metaphorical tapping shoes and get ready to dance through life with less stress and more joy!
Environmental Issues
The world around us isn’t just a delightful backdrop for our Instagram photos; it plays a significant role in the health saga of humanity. Environmental factors contribute to the prevalence of chronic diseases, often lurking like a villain in a superhero movie, making their presence felt when least expected. From air pollution to chemical exposure, the environment can be a sneaky saboteur to our health, demonstrating that nature isn’t always the gentle giant we hope it to be.The link between chronic diseases and environmental factors is more evident than ever.
Numerous studies have shown that pollution, poor urban planning, and climate change can exacerbate conditions like asthma, heart disease, and diabetes. A breath of fresh air? Not so much, especially if that air is thick with smog. According to the World Health Organization, approximately 7 million people die each year due to environmental factors, making it clear that clean air and water are not just luxuries; they are necessities for a healthy life.
Strategies for Reducing Environmental Risks to Health
Addressing environmental risks to health requires a multi-faceted approach as complex as deciphering the plot of a Christopher Nolan film. Here are some strategies that have been effective in tackling these issues:
- Improving Air Quality: Governments can implement stricter regulations on emissions from vehicles and factories. The Clean Air Act in the United States has showcased how concerted efforts can lead to a significant reduction in air pollutants.
- Promoting Green Spaces: Urban areas can benefit immensely from parks and green spaces. These not only help improve air quality but also provide communities with recreational areas that promote physical activity and mental well-being.
- Encouraging Sustainable Practices: Initiatives that promote recycling, composting, and reducing single-use plastics can help reduce waste and pollution. Countries like Sweden have taken significant strides, aiming to be carbon neutral by 2045.
- Raising Public Awareness: Educational campaigns can help individuals understand the impact of their choices. For example, the “Plastic Free July” initiative encourages people to reduce plastic use, leading to a collective decrease in waste generation.
The importance of these strategies cannot be overstated. By implementing these initiatives, communities not only work towards a healthier environment but also invest in the long-term health of their populations, effectively turning the tide against chronic diseases related to environmental factors.
Successful Public Health Initiatives Addressing Environmental Issues
There have been noteworthy public health initiatives that successfully tackled environmental issues head-on, creating a blueprint for future efforts. Here are a few shining examples:
- The Clean Water State Revolving Fund: This U.S. program provides financial assistance to improve water quality, demonstrating that clean drinking water is crucial for community health. A well-hydrated community is a happy community!
- The Urban Heat Island Project: In cities like Los Angeles, initiatives to plant trees and increase vegetation have been implemented to combat rising temperatures, thereby reducing heat-related illnesses and improving overall air quality.
- Lead Poisoning Prevention Programs: Targeted efforts in cities like Flint, Michigan, have focused on improving infrastructure and educating residents about lead exposure, turning a crisis into an opportunity for community engagement and health advocacy.
These initiatives provide a glimpse of what can be achieved when public health is prioritized, showing that a little investment in the environment can yield significant health dividends. Remember, a clean environment is not just a nice-to-have; it’s a fundamental requirement for a thriving society!
Health and Ergonomics
Ergonomics, the science of designing the workplace to fit the user, is not just about making things look pretty; it’s about preventing chronic pain and musculoskeletal disorders that can turn even the most enthusiastic worker into a grumpy potato. Think of it as giving your body a comfy chair at the table of life, instead of making it sit on a hard stool that screams, “Get up and stretch!” every five minutes.Proper ergonomics can drastically reduce the risk of chronic pain and injuries.
When your workstation is set up correctly, it minimizes the strain on your body, allowing for a happier and healthier you. A well-designed workspace not only enhances productivity but also keeps your body from feeling like it’s been through an 18-hour dance marathon.
Ergonomic Solutions for Home and Workplace Settings
Creating an ergonomic workspace is crucial for anyone who spends long hours sitting. Here are some solutions that will make your home or office feel like a spa retreat for your body:
1. Chair Matters
Invest in a chair that offers lumbar support. It should feel like a warm hug for your back, keeping you aligned and cozy.
2. Desk Height
Your desk should be at a height where your elbows are at a 90-degree angle when typing. If you feel like a troll hunched over a cave, it’s time to adjust!
3. Monitor Position
Place your monitor at eye level and about an arm’s length away. If you’re straining your neck like a giraffe trying to see the top of a tree, you need to lower it!
4. Keyboard and Mouse
Keep your keyboard and mouse close enough that you don’t have to reach – we’re not training for the Olympics here!
5. Frequent Breaks
Stand up, stretch, and do the office chair cha-cha every 30-60 minutes. Your body will thank you for those mini dance breaks!
“An ounce of prevention is worth a pound of cure.” – Benjamin Franklin, probably after a long day of writing
In summary, ergonomic furniture and practices can transform a torturous workhorse into a comfort zone, giving your body a fighting chance against the evils of poor posture and repetitive strain. Your future self will give you a high five for it!
Health and Exercise
Regular exercise is like that enthusiastic friend who always shows up uninvited to parties—only this time, it’s a party for your health! Engaging in physical activity is essential in managing chronic diseases, as it helps to improve overall well-being, boost mood, and even reduce the intensity of symptoms. Whether you’re a couch potato or a workout warrior, there’s always room to lace up those sneakers and get moving!The benefits of regular exercise in managing chronic diseases are backed by science, and let’s face it, who doesn’t want to be the star of their own health improvement story?
Exercise can lead to better circulation, improved metabolic function, and even more manageable symptoms for conditions like diabetes, arthritis, and heart disease. It’s not just about sweating it out—it’s about bringing joy and mobility back into life.
Workout Plans for Individuals with Chronic Conditions
Understanding that each individual is unique, workout plans can be tailored to fit various chronic conditions. Here’s a selection of workout plans that cater to different needs, ensuring that everyone can join the fitness fiesta!
1. Low-Impact Aerobics
Ideal for those with joint issues or arthritis.
Duration
30 minutes
Frequency
3-5 times a week
Activities
Swimming, cycling, or walking at a moderate pace.
2. Strength Training
Perfect for individuals looking to build muscle without overexertion.
Duration
20-30 minutes
Frequency
2-3 times a week
Activities
Light weights or resistance bands focusing on major muscle groups.
3. Flexibility Exercises
Great for improving mobility and decreasing stiffness.
Duration
15-20 minutes
Frequency
Daily
Activities
Yoga or gentle stretching routines.
4. Balance Training
Best for those prone to falls or with neurological conditions.
Duration
10-15 minutes
Frequency
2-3 times a week
Activities
Tai Chi or stability exercises like standing on one leg.For all the plans above, it’s crucial to warm up before starting and cool down afterward. Think of it as preparing your body for a mini-adventure and then helping it unwind afterward!
“Exercise is a celebration of what your body can do, not a punishment for what you ate.”
Success Stories of Improved Health Through Exercise
Let’s sprinkle some inspiration on this topic with success stories that prove the potency of exercise in transforming lives.
Tom’s Triumph Over Diabetes
Tom, a 55-year-old with Type 2 diabetes, decided to trade his sofa for sneakers after realizing that his blood sugar levels were dancing a little too much. After committing to a routine of brisk walking and strength training, he not only lowered his A1C levels but also lost 30 pounds! Tom now runs 5K races and has become a local ambassador for fitness.
Linda’s Journey with MS
Linda, diagnosed with multiple sclerosis, found herself struggling with fatigue and muscle weakness. By incorporating yoga and balance training into her routine, she discovered newfound energy levels and improved her coordination. Her favorite part? Showing off her yoga poses on social media, inspiring others with her journey!
Kevin’s Comeback from Heart Disease
After a heart attack, Kevin knew he needed to change his lifestyle. He started with doctor-approved light exercises and gradually built up to cycling and swimming. Now, he participates in charity cycling events, proving that it’s never too late to pedal your way back to health.These stories highlight that exercise can indeed be a game-changer in the management of chronic diseases.
It’s about finding joy in movement and celebrating every small victory along the way!
Eyes
In the grand scheme of life, our eyes are like the windows to our soul—only way more prone to chronic diseases! Just like any other part of our body, our peepers can encounter a variety of pesky conditions that can dramatically shatter our visual delights. Chronic eye diseases, such as glaucoma, macular degeneration, and diabetic retinopathy, can not only cloud our vision but also dim our quality of life.
Imagine trying to enjoy a good book or surf the web when everything just looks like a Picasso painting—chaotic and misplaced!Chronic eye diseases can lead to significant impairments, affecting not just our sight but also our independence and overall mental health. With around 2.7 million people in the U.S. alone suffering from glaucoma, it’s clear that maintaining eye health is no laughing matter—yet we can still chuckle at our attempts to read without our glasses.
Preventive measures and treatments are crucial in keeping our eyes sparkling and sharp.
Chronic Eye Diseases and Their Impact
Chronic eye diseases impact daily activities and overall quality of life in various ways. Here are some significant effects:
- Limited independence: Losing vision can make simple tasks like cooking or driving feel like an obstacle course designed by an evil mastermind.
- Increased risk of accidents: Reduced vision can lead to accidents and falls, making the world feel like a minefield—watch out for that coffee table!
- Emotional toll: The stress of coping with vision loss can lead to anxiety and depression, turning happy-go-lucky folks into sad sack couch potatoes.
- Social isolation: Difficulty seeing can hinder social interactions, causing some to retreat into their own bubble, likely filled with cats and knitting supplies.
Protecting our vision on a daily basis is essential for warding off these unfortunate changes. Luckily, light is at the end of the tunnel, and it doesn’t involve a train!
Preventive Measures and Treatment Options
Maintaining eye health is not just a task; it’s a lifestyle! Here are some effective strategies to keep those orbs functioning at their best:
- Regular eye exams: Visits to the optometrist are key. Think of them as your vision’s personal trainer—without the sweat and inspirational quotes.
- Healthy diet: Foods rich in vitamins A, C, and E, as well as omega-3 fatty acids, can boost eye health. So, eat those carrots, spinach, and fish like they’re going out of style!
- Protective eyewear: Sunglasses aren’t just a fashion statement; they protect against harmful UV rays. Rock those shades like a superstar!
- Manage chronic conditions: Keeping diabetes and hypertension in check can prevent complications like diabetic retinopathy. Control those numbers like a seasoned accountant!
Maintaining vision protection during everyday activities can also make a world of difference. Here are some helpful tips:
Vision Protection in Everyday Activities
Keeping your vision safe doesn’t have to be a full-time job. Here are everyday strategies worth incorporating:
- Good lighting: Ensure your living and working environments are well-lit to reduce strain. Think of it as setting the perfect mood—just without the romantic music.
- Screen breaks: Follow the 20-20-20 rule: every 20 minutes, look at something 20 feet away for 20 seconds. Your eyes will thank you, and you might discover your cat plotting world domination!
- Hydration: Drink plenty of water to keep the eyes lubricated. It’s like giving your eyes a refreshing spa day—minus the cucumbers.
- Exercise: Regular physical activity can lower the risk of chronic eye diseases. So, get moving—there’s a reason those treadmill commercials are so persuasive!
Fitness Equipment
In the grand quest for fitness while managing chronic diseases, the right equipment can be your trusty sidekick. Think of fitness gear as the magical tools in your superhero utility belt, but instead of fighting crime, they help you tackle health challenges! With the right pieces, you can turn your living room into a battleground against sedentary habits, all while wearing those comfy sweatpants you love.Essential fitness equipment for individuals managing chronic diseases includes a variety of tools that cater to different abilities and workout preferences.
Whether it’s a simple yoga mat or a more complex resistance band, each piece plays a vital role in promoting a healthier lifestyle. Let’s dive into the essential items and some tips on how to use them safely and effectively.
Essential Fitness Equipment
Creating a safe and effective workout space starts with understanding which equipment will best support your unique health needs. Here’s a list of recommended essentials:
- Resistance Bands: Perfect for those who need low-impact options, these stretchy wonders help build strength without the bulk of weights.
- Yoga Mat: A must-have for floor exercises, stretching, and stability. Choose one with good grip to prevent any slip-ups – we want you to flow, not flop!
- Dumbbells: Ideal for strength training; start light and gradually increase weight as strength improves. Remember, it’s about progress, not the Hulk transformation overnight!
- Stationary Bike: Great for cardio workouts that are easy on the joints. Put on your favorite tunes or a podcast and pedal your way to fitness while simultaneously mastering the art of multitasking.
- Foam Roller: For post-workout relaxation and muscle recovery, this handy tool helps ease tension and soreness. Think of it as a personal masseuse that doesn’t charge by the hour!
Guidelines for Safe and Effective Use of Fitness Equipment
Using fitness equipment safely is paramount, especially for individuals with chronic diseases. Here are some guidelines to keep you on the right path:
- Always warm-up before workouts to prep your muscles and reduce injury risk. Five minutes of gentle movement can work wonders!
- Focus on form over speed. It’s better to do a few reps correctly than to rush through and risk hurting yourself. Remember, slow and steady wins the fitness race!
- Listen to your body. If something doesn’t feel right, it’s okay to take a break or modify the exercise. Your body is like a finely-tuned musical instrument; don’t play it out of tune!
- Stay hydrated! Keep a water bottle nearby and sip regularly. Hydration is your body’s best friend during any workout adventure.
- Consider consulting a fitness professional or physical therapist to tailor a program that fits your specific health needs and to ensure you’re using equipment correctly.
Creating a Home Workout Space
Transforming a nook in your home into a dedicated workout space can make all the difference in staying motivated. Here’s how to do it:
- Choose the Right Location: Pick a spot with enough room to move around freely. A corner in the living room or a quiet area in the basement can work wonders.
- Keep It Organized: Use baskets or storage bins to keep your equipment tidy and accessible. A clutter-free area promotes a clutter-free mind!
- Add Personal Touches: Hang motivational quotes or photos to inspire you. A little pizzazz goes a long way in making your space feel welcoming.
- Ensure Good Lighting: Natural light is best to keep your spirits high! If that’s not an option, consider bright, warm lights to keep the energy flowing.
- Have a Workout Playlist Ready: Music can turn a mundane workout into a dance party! Create a playlist that pumps you up and keeps you moving.
Final Wrap-Up
As we wrap up this journey through the ups and downs of Chronic diseases, remember that knowledge is power, and a healthy lifestyle is the ultimate plot twist! Whether it’s embracing exercise, making better food choices, or finding a supportive community, there’s always a way to navigate these health hurdles. So, let’s take this newfound wisdom, share a laugh or two, and tackle chronic diseases with the gusto of a superhero on a mission!
Essential Questionnaire
What are chronic diseases?
Chronic diseases are long-lasting conditions that usually cannot be cured but can be managed through lifestyle changes and medical treatment.
How can lifestyle choices affect chronic diseases?
Poor diet, lack of exercise, and smoking can increase the risk of developing chronic diseases, while healthy habits can help manage or even prevent them.
Can chronic diseases be cured?
Most chronic diseases cannot be cured but can often be controlled with proper management and lifestyle adjustments.
How important is early detection of chronic diseases?
Early detection is crucial as it can lead to better management and improved quality of life, reducing the risk of complications.
Are there support systems for individuals with chronic diseases?
Yes, there are various support groups and resources available for individuals dealing with chronic diseases, including counseling, medical support, and community programs.